From Diagnosis to Treatment: The Impact of AI on Rare Disease Drug Development
Drug development for rare (also referred to as orphan) diseases is notoriously challenging. Legislative initiatives, such as the 1983 US Orphan Drug Act and 1999 EU Orphan Regulation, provide regulatory and economic incentives to drug developers. Despite an increase in the number of annually FDA-approved drugs with an orphan designation from 2 in 1983 to 33 in 2020, more than 90% of rare diseases still lack effective therapies.
With an estimated 7,000 rare diseases affecting around 350 million people worldwide, the space presents a huge untapped potential, but the scarcity of patients affected by each disease poses significant hurdles to biotech and pharma companies aiming to develop rare disease treatments. Artificial intelligence and machine learning (AI / ML) have been the buzz in biotech and pharma for a couple of years now, promising faster, cheaper, and overall more successful drug development. Given their capacity to sift through and detect pattern ins large datasets (be it diagnostic images, genomic info, patient records, or scientific literature), AI algorithms might be uniquely suited to bridge the information gaps in the rare disease space. Indeed, a number of biotech and pharma players are beginning to harness the power of artificial intelligence to address various pain points of drug development for rare diseases.
Drug discovery
Classical models of drug discovery and development, with development times of over a decade and failure rates averaging in the range of 90%, might not be well-suited for the rare disease space. Innovative approaches to drug discovery could help to shorten the time to the clinic and further derisk clinical candidates with corroborating disease information.
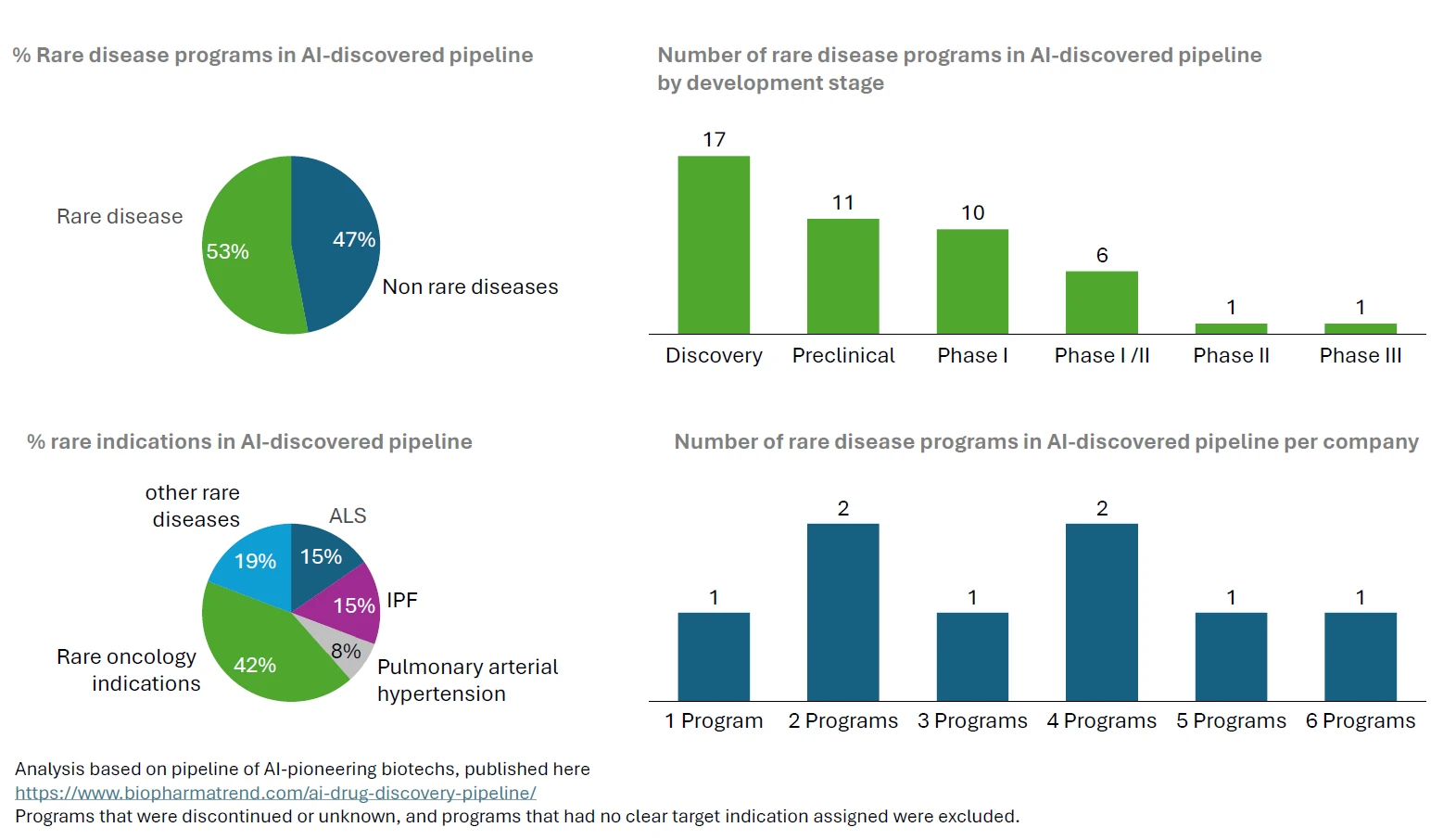
Among a group of AI-pioneering biotechs that center their target discovery and molecule design platforms around AI-driven engines, 8 out of 9 included rare disease candidate treatments as part of their portfolio and around half of the 49 AI-discovered programs targeted rare diseases. The most common rare indications were amyotrophic lateral sclerosis (ALS), a progressive disease of the CNS that involves the loss of muscle control and is eventually fatal and idiopathic pulmonary fibrosis (IPF), a chronic lung disease that causes progressive and irreversible decline in lung function, with a median survival of only 3 to 4 years. Several players also targeted other rare diseases including different types of rare cancers.
Among the clinically most advanced AI-discovered molecules in the rare disease space are Recursion’s fast-tracked HDCA inhibitor REC-228 for treatment of NF2-Mutated Meningiomas and insilico’s INS018_055, a small molecule TNIK inhibitor in Phase II trials for IPF. Insilico’s molecule received FDA orphan designation in 2023. Two of Recursion’s rare disease candidates also received Orphan designation, REC-994, a small molecule superoxide scavenger developed for the treatment of Cerebral Cavernous Malformation, and the MEK inhibitor REC-4881 for the treatment of Familial Adenomatous Polyposis. Both drugs candidates are currently in Phase II trials.
ALS, a high unmet need rare neurological indication, is another focus of AI-pioneering biotechs. Verge Genomics’s VRG50635, a small molecule PIKfyve inhibitor, was found safe in healthy volunteers and is being tested in a recently initiated proof of concept study. Other AI-discovered candidate treatments for ALS include Benevolent AI’s retinoic acid receptor alpha-beta agonist that is currently in preclinical development, as well as insitro’s and Verge’s (Lilly-partnered) discovery programs.
Next to these approaches to enhance target and molecule discovery with AI, other players aim to accelerate the availability of rare disease treatments by repurposing existing drugs. For example, Healx's Healnet platform combines various rare disease data sources into a knowledge graph that uncovers promising disease-compound relationships. Similarly, nonprofit Every Cure, works on a three-year project aiming to find rare disease drugs by AI-driven drug-repurposing and recently received a $48 million in funding from the Advanced Research Projects Agency for Health.
Diagnostics
Many rare disease patients undergo a diagnostic odyssey, waiting years until they receive the correct diagnosis for their disease, which impacts patients’ quality of life, but also impedes the clinical testing of novel drugs.
An estimated 80% of rare diseases have a genetic component, making them prime targets for genetic diagnosis. Fueled by improvements and increased cost-effectiveness of next-generation sequencing, a wealth of genomic data is now available with an expanding catalog of variants in ~4000 genes with ~6500 diseases and their annotated phenotypes. However, among the massive body of genomic information, it can be challenging to manually pinpoint disease-causing candidate variants in large-scale datasets, and evidence for pathogenic variants might not be available in all biobanks.
AI / ML algorithms that quickly sift through massive amounts of data, such as those developed by Berlin-based Nostos Genomics and US company Genomenon could help streamline genomic interpretation processes and thus expedite diagnosis. However, as for any AI application, the algorithm is only as good as the input data, and limitations that arise from biases in genomic datasets need to be considered when developing AI-driven diagnostic algorithms in the rare disease field.
Next to helping clinicians to rapidly identify disease-causing variants, AI-based models could also allow integrating various other data sources, from patient records to multi-omics datasets. This also includes phenotypic information, such as facial features, which can be indicative of rare disease phenotypes. Algorithms such as ClinFace help clinicians diagnose disease based on 3D facial images of their patients.
An interesting approach for linking genotypic data to rare disease phenotypes is taken by genetics service provider FDNA. In an approach that they coin next-generation phenotyping (NGP),FDNA’s AI platform integrates facial features with genetics data from over 10,000 diseases to increase the diagnostic accuracy of rare diseases.
Clinical trials
Conducting randomized clinical trials is often not feasible for rare diseases due to challenges that relate to the small number of patients and lack of information on biomarkers and trial endpoints.
AI-based solutions could help address those challenges in clinical development in the rare disease space, by tailoring trial designs, identifying relevant biomarkers and surrogate endpoints from patient data, improving patient recruitment, implementing Real World Evidence (RWE) / Real World Data (RWD), and streamlining data analysis.
Service provider companies such as IPM.ai are using AI-driven exploration of RWD to find rare disease patients for contribution in clinical trials and for commercialization. AI could also help patients, or their caretakers find trials. In the rare disease field, patients and their families are often disease experts by necessity and take a great part in organizing treatment and care. Tools such as TrialGPT, developed by Jimeng Sun’s lab at the University of Illinois in collaboration with the US NIH, could allow patients to prompt a large language model to find and rank appropriate trials.
Acknowledging the challenge of clinical development with a small number of patients, regulatory agencies explore possibilities to enhance the utility of RWE / RWD for clinical research in rare diseases, though open questions remain on RWE data quality, privacy, and standardizations. Generally, AI could help to fill data gaps in rare disease trials, for example by integrating real-world evidence-based control arms. Digital twins, as proposed by San Francisco-based startup Unlearn, could reduce the number of patients needed for a trial. Digital twin-based placebo or comparator groups could be especially beneficial for rare diseases with severe phenotypes, in which the use of placebo might be unethical. To overcome challenges of sparse data, also raising concerns about patient anonymity, new models such as federated learning could pave the way towards collaborations that make the best use of the data available in the rare disease space.
AI-driven technologies could also help mitigate the logistical challenges common to clinical trials in the rare disease space, with often geographically dispersed clinical sites. Saama, a software company based in California, employs AI to assist organizations in automating various aspects of clinical trials by centralizing data collection, storage, and access, enabling real-time collaboration among stakeholders. AI-driven monitoring systems, including data readouts from wearables as well as AI-powered Chatbots that bridge communication between patients and researchers, could take decentralized trials to the next level.
While holding great potential, AI-aided improvements of clinical trials for rare disease are currently less advanced than tools for molecule discovery and diagnosis. However, the recent uptake in generative AI and user-friendly large language models, will likely spawn new applications to make clinical trials in rare diseases more efficient and patient-centric.
Conclusion
The industry is increasingly using AI / ML to address the unique challenges of drug development in rare diseases, a trend that is expected to increase as AI applications move towards the mainstream of drug development. This coincides with increased public interest in innovation in the rare disease space, reflected in regulatory initiatives like Operation Warp Speed initiative for rare disease treatments and allocation of government funding for AI-driven drug finding for rare diseases. However, challenges inherent to the field, such as scarcity and sparseness of patient data, concerns about data privacy and patient anonymity, and lack of AI explainability, could impede further uptake. Educating key stakeholders on the potential but also the shortcomings of AI will be vital for the broader acceptance of AI technology as a pillar of drug development within the tight-knit rare disease community.
Topics: AI & Digital